Ineffective Esophageal Motility Isocontour Analysis
Ineffective Esophageal Motility Manometric Isocontour Analysis: Spatiotemporal Differences from Healthy Controls
Ineffective esophageal motility (IEM) has been defined by derived pressure metrics of distal smooth muscle esophageal contractile integral. Due to the large variability of manometric data, spatiotemporal characterization of the entire deglutitive esophageal body pressure isocontour and comparison of IEM to healthy controls requires numerous normalized isocontour maps to discern differences. Thus, we seek to establish the feasibility of an aggregate normalized isocontour database to: 1) Evaluate deglutitive esophageal isocontours for mean (the average pressure isocontour) as well as the variance of pressure magnitudes (the standard deviation (SD) isocontour) in healthy controls and IEM patients diagnosed by Chicago Classification metrics. 2) Over the entire isocontour, statistically compare and display the times and regions of significant pressure differences between healthy controls and IEM patients. We studied 1800 swallows across 52 healthy subjects (50±14 yrs,20F) and 128 IEM patients (57±15, 71F) using high resolution manometry. Manometric data were obtained from the ManoBank. IEM patients were defined using the Chicago Classification criteria. All subjects performed 5 ml water swallows (x10). Each swallow was normalized by defining “time zero” as the instant of initial deglutitive upper esophageal sphincter (UES) relaxation and by defining the inter-sphincteric esophageal length. In addition to characterizing average and SD, disease-related differences in isocontours were tested using analysis of variance spanning the entire isocontour across all subjects.
Average and SD isocontours showed that average peristalsis (top row of graphs in figure 7) is subtly different for control and IEM groups. These differences are 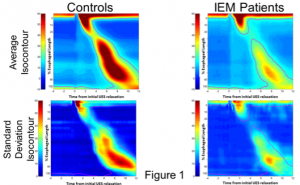 further clarified by the SD isocontours (lower row of graphs, figure 7) wherein IEM swallows showed less robust distal esophagus contractility. Control group swallows showed variability in both the proximal and distal esophagus whereas variability was confined more to the distal esophagus in IEM patients. The significant group-wise effects are shown in figure 8
further clarified by the SD isocontours (lower row of graphs, figure 7) wherein IEM swallows showed less robust distal esophagus contractility. Control group swallows showed variability in both the proximal and distal esophagus whereas variability was confined more to the distal esophagus in IEM patients. The significant group-wise effects are shown in figure 8 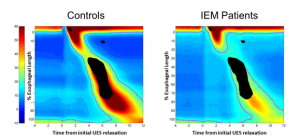 where regions of significant difference (p<0.0001, corrected for multiple comparisons) are overlaid in black on the average isocontour maps in both groups and are seen in the distal esophagus and in the pressure fall-out region of the esophagus (aka “transition zone”).
where regions of significant difference (p<0.0001, corrected for multiple comparisons) are overlaid in black on the average isocontour maps in both groups and are seen in the distal esophagus and in the pressure fall-out region of the esophagus (aka “transition zone”).
In conclusion, differences in esophageal motility in IEM patients compared to controls are primarily in the distal esophagus and transition zone.
